It is unsurprising, therefore, that Si is now an integral part of regenerative bone materials. The implications of this are not yet clear although it is understood that (i) men, post-menopausal women taking hormone replacement therapy and pre-menopausal women, show a positive relationship between dietary Si intakes and bone mineral density (BMD), and (ii) when growing rats were supplemented with a highly bioavailable form of dietary Si (namely monomethylsilanetriol) their increase in Si status, adjudged from fasting serum Si levels, positively correlated with their increase in BMD. revealed that bone mineral can vary quite markedly, by about an order of magnitude, in its Si content. Furthermore, in contrast to bone collagen Si levels, which have been shown to be constant regardless of total bone Si-levels, Jugdaohsingh et al. Recently identified mammalian Si transporters may enable this Si conservation. For example, a relatively recent study showed that bone retains its Si content even with imposed dietary deprivation rats, stressed in this way, shut down Si excretion in urine and appear to conserve their already acquired Si for connective tissue function, while still displaying a relatively normal phenotype. While the precise role of Si in bone tissue has yet to be determined, there are a number of important observations that have been made. Subsequent work, which has frequently been hampered by the difficulty in achieving truly Si-free diets, has shown smaller, but significant changes in bone structure such as a reduction in both the phosphate content of bone and the tibia growth plate thickness in Si-deprived animals. The earliest studies of Carlisle and Schwarz showed dramatic detrimental changes in the structure of bone and collagenous tissues, such as skull deformities in rats and absent wattles and combs in chicks, when dietary Si deprivation was induced. The impact of this dietary Si appears to be a positive effect on connective tissue growth and maintenance. Various studies have shown that it is the soluble OSA component, either from direct ingestion or following digestion in the gut, that is readily absorbed, rapidly increasing serum Si levels. Furthermore, we show that this substitution, at the low silicate concentrations found in the biological environment, is likely to be a driver of calcium phosphate crystallization from an amorphous to a fully mineralized state.ĭietary silicon (Si) intake, estimated at 20–50 mg ingested person −1 d −1 in the western world, largely comes in the form of digestible phytolytic silica from plants (primarily cereals) and as orthosilicic acid (OSA), a weak acid with a pKa of 9.8, in fluids such as drinking water. Formation energy analysis revealed that OSA is not favourable as a neutral interstitial substitution but can be incorporated as a silicate ion substituting for a phosphate ion, suggesting that incorporation will only occur under specific conditions at the bone-remodelling interface and that dietary forms of Si will be metabolized to simpler chemical forms, specifically SiO 4 4 −. 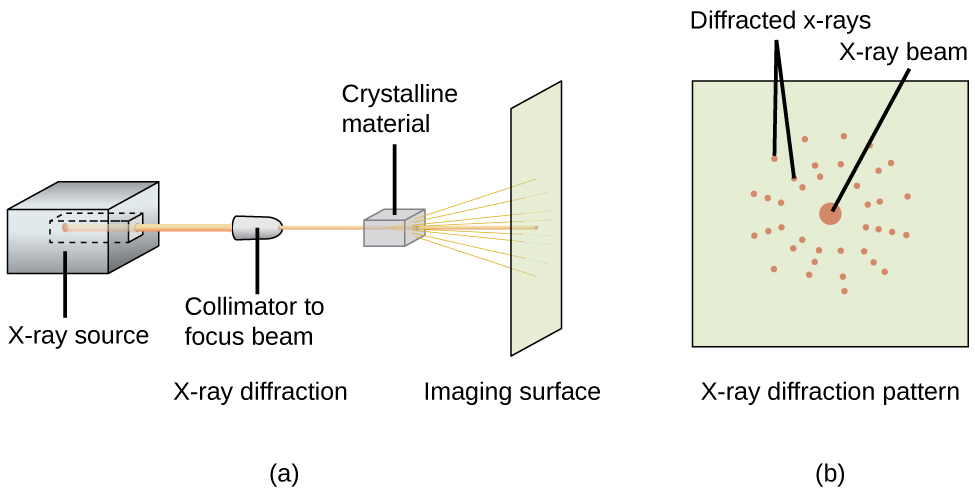
Thus we used first principles density functional theory calculations to explore the energetic and geometric consequences of substituting OSA into a large HA model. However, theoretical XRD patterns revealed that at the levels found in bone, the ‘Si effect’ would be virtually undetectable. X-ray diffraction (XRD) of rat tibia bone mineral showed that the mineral phase was similar to that of phase-pure HA. In this study, given Si's recognized positive effect on bone growth and integrity, we examined the chemical form and position of this natural Si source in the inorganic bone mineral hydroxyapatite (HA). Under physiological conditions, the predominant form of bioavailable silicon (Si) is orthosilicic acid (OSA).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
